A rhythm within a rhythm | ECG challenge #7
These ectopic beats look familiar. But something doesn't add up.
The case
A 58-year-old man has a routine health check. He has no symptoms. He has a history of hypertension managed with lisinopril.
His blood pressure is 142/88 mmHg, and pulse is 72 bpm. Heart sounds are normal.
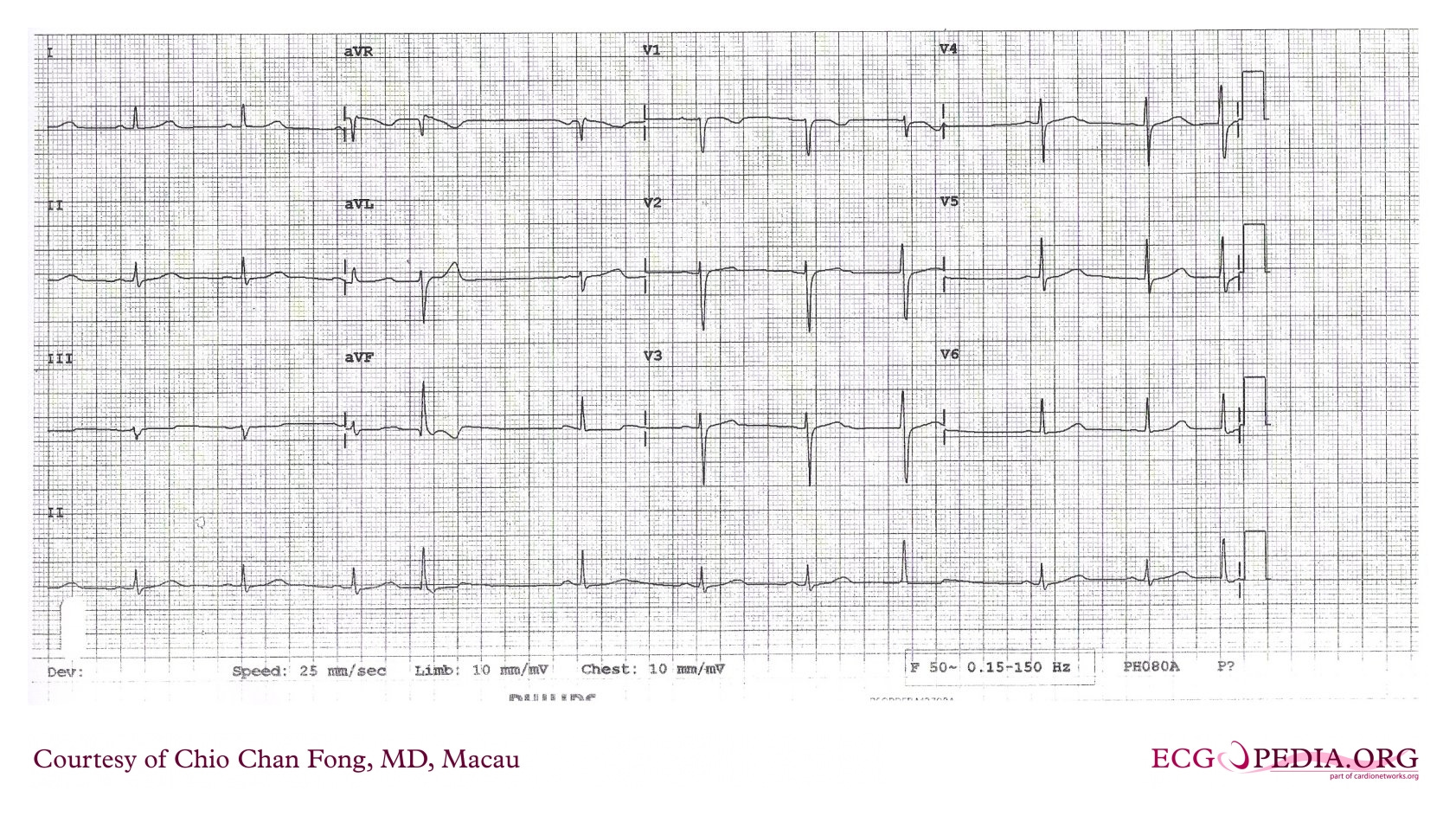
A 12-lead ECG is performed.
ECG systematic analysis
Paper speed: 25 mm/s and voltage: 10 mm/mV (confirmed on printout).
This ECG shows the following:
Rhythm: Sinus rhythm with intermittent ectopic beats. The ectopic beats are monomorphic. The coupling intervals between sinus beats and ectopic beats vary.
P waves: ~70 bpm, normal axis (positive in lead II, negative in aVR). Normal duration and voltage.
PR interval: Normal.
QRS complex:
Rate: Variable (including ectopic beats).
Duration: Less than 120 ms for sinus beats. Borderline (~120 ms, possibly less) for ectopic beats.
Axis: Normal for sinus beats (positive in leads I and II).
Morphology: Normal and narrow in sinus beats. The ectopic beats are wider, monomorphic, with higher voltage than sinus beats and no consistent preceding P wave.
QT interval: Normal on sinus beats, though difficult to assess accurately due to the intermittent ectopic beats.
ST segment: No significant changes in sinus beats.
T waves: Normal in sinus beats.
Overall, sinus rhythm with intermittent monomorphic ectopic beats at variable coupling intervals, consistent with parasystole.
Note: the fifth QRS complex in the bottom rhythm strip is an ectopic beat that appears to be preceded by a P wave. This is most likely a sinus P wave that coincided with the ectopic focus firing. The ectopic beat has the same QRS morphology as the other ectopic complexes, confirming it was driven by the ectopic focus, not by the sinus impulse.
Correct answer
Parasystole.
Most people look at this ECG and see premature complexes, probably PVCs. They’re not wrong to notice ectopic beats. But look again at the coupling intervals: the time between each preceding sinus beat and the following ectopic beat is different every time. That’s not how premature beats behave.
Ordinary premature beats have fixed coupling intervals. The ectopic focus fires at a set time after the preceding sinus beat, usually through a re-entrant or triggered mechanism that depends on the sinus depolarisation to initiate it. Measure the coupling interval once, measure it again on the next premature beat, and you get more or less the same number.
Parasystole is fundamentally different. It’s a second clock running inside the heart, completely indifferent to what the sinus node is doing:
An ectopic focus (a secondary pacemaker) fires in parallel with the SA node through its own spontaneous automaticity.
Its intrinsic rate is typically slower than the sinus rate (though not always).
The focus is protected by entrance block: the surrounding tissue has depressed conduction that blocks incoming impulses, so the sinus rhythm can’t reset or suppress it. The focus can propagate its impulse outward and depolarise the ventricles, but nothing from outside can penetrate in.
Occasionally, there is also exit block: the ectopic impulse fires, but the surrounding myocardium is still refractory, so the impulse can’t escape.
Three diagnostic criteria follow directly from this one mechanism. All three are visible on a 60-second lead II rhythm strip from the same patient:
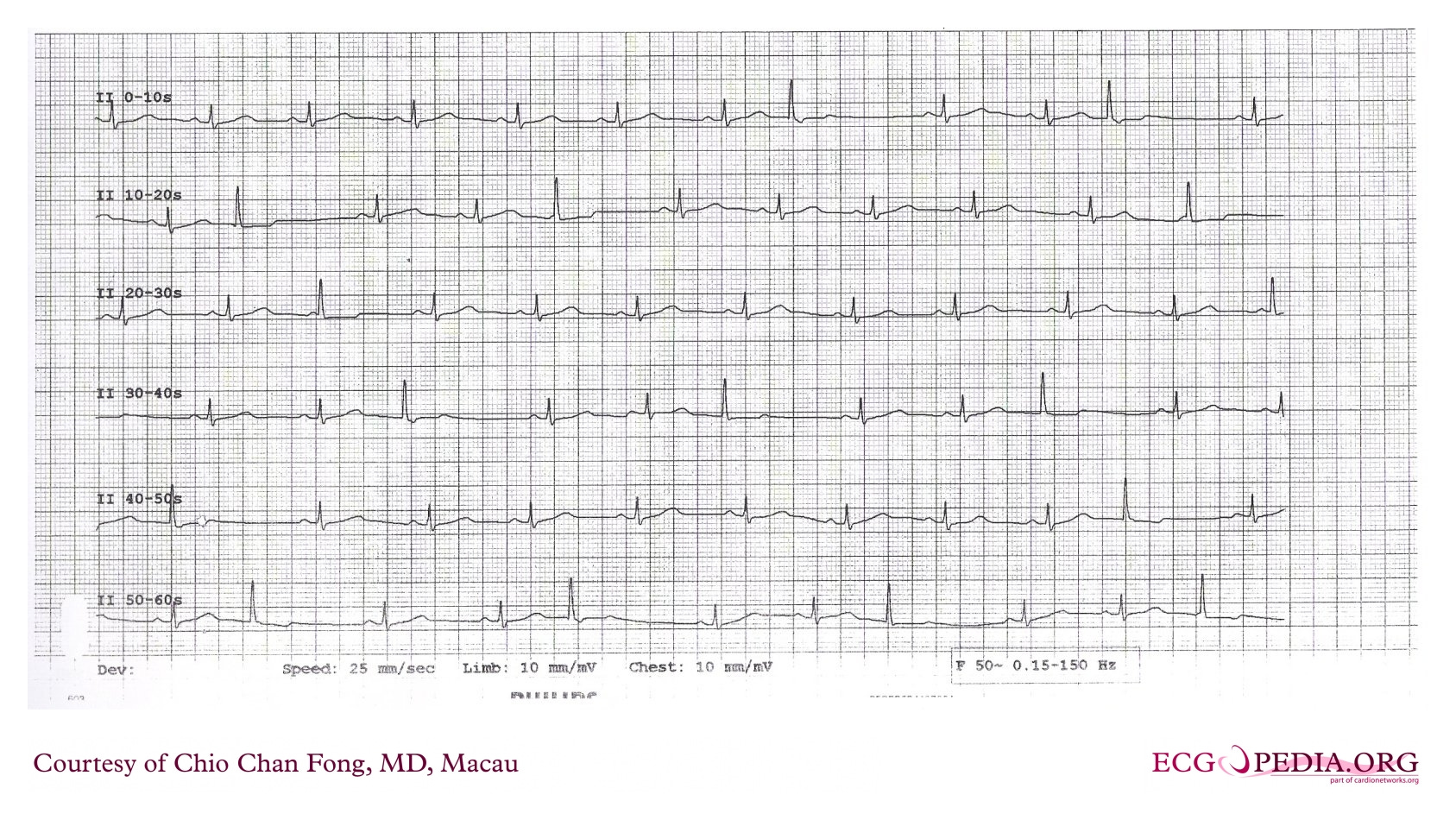
1. Interectopic intervals are multiples of a common denominator. If the ectopic focus really is an independent clock, it fires at a fixed cycle length (call it X). The intervals between consecutive visible ectopic beats should all be multiples of X (1X, 2X, 3X…). They are.
On the annotated strip below, vertical lines mark each ectopic firing: blue solid lines where the impulse successfully depolarised the ventricles, and red dashed lines where it fired but couldn’t escape (exit block). The gaps between visible beats vary, but every one is a close multiple of the same base interval X (small variations in the ectopic firing rate are normal and expected).
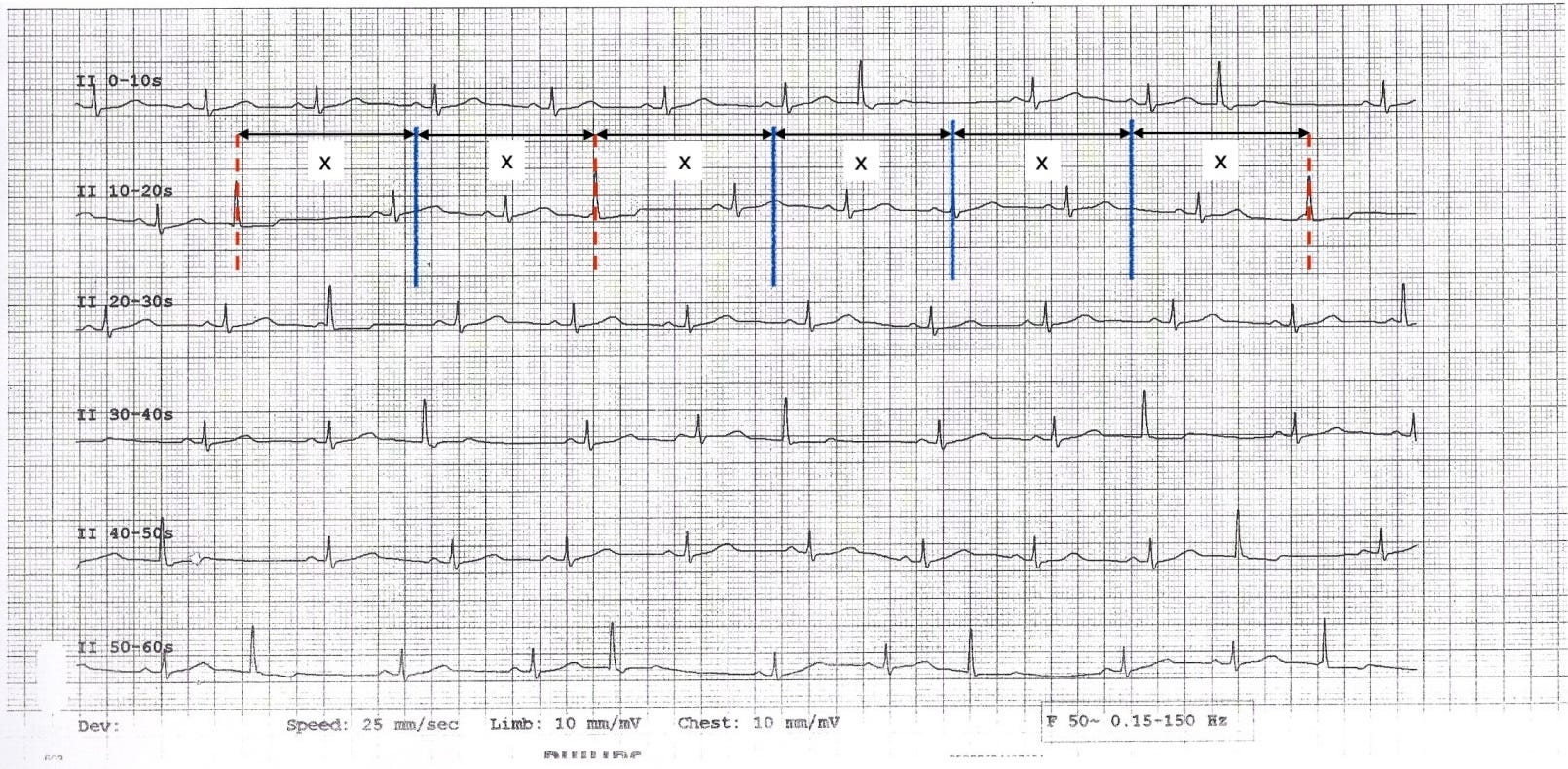
2. Variable coupling intervals. Because the ectopic focus fires on its own schedule, the gap between a sinus beat and the next ectopic beat depends entirely on where in the ectopic cycle the sinus beat happened to fall.
On the annotated strip below, two coupling intervals are marked: "y" (red arrow, first strip) and "z" (blue arrow, fourth strip). They are visibly different lengths. This is the feature that distinguishes parasystole from ordinary premature ectopic beats, where the coupling interval is fixed.
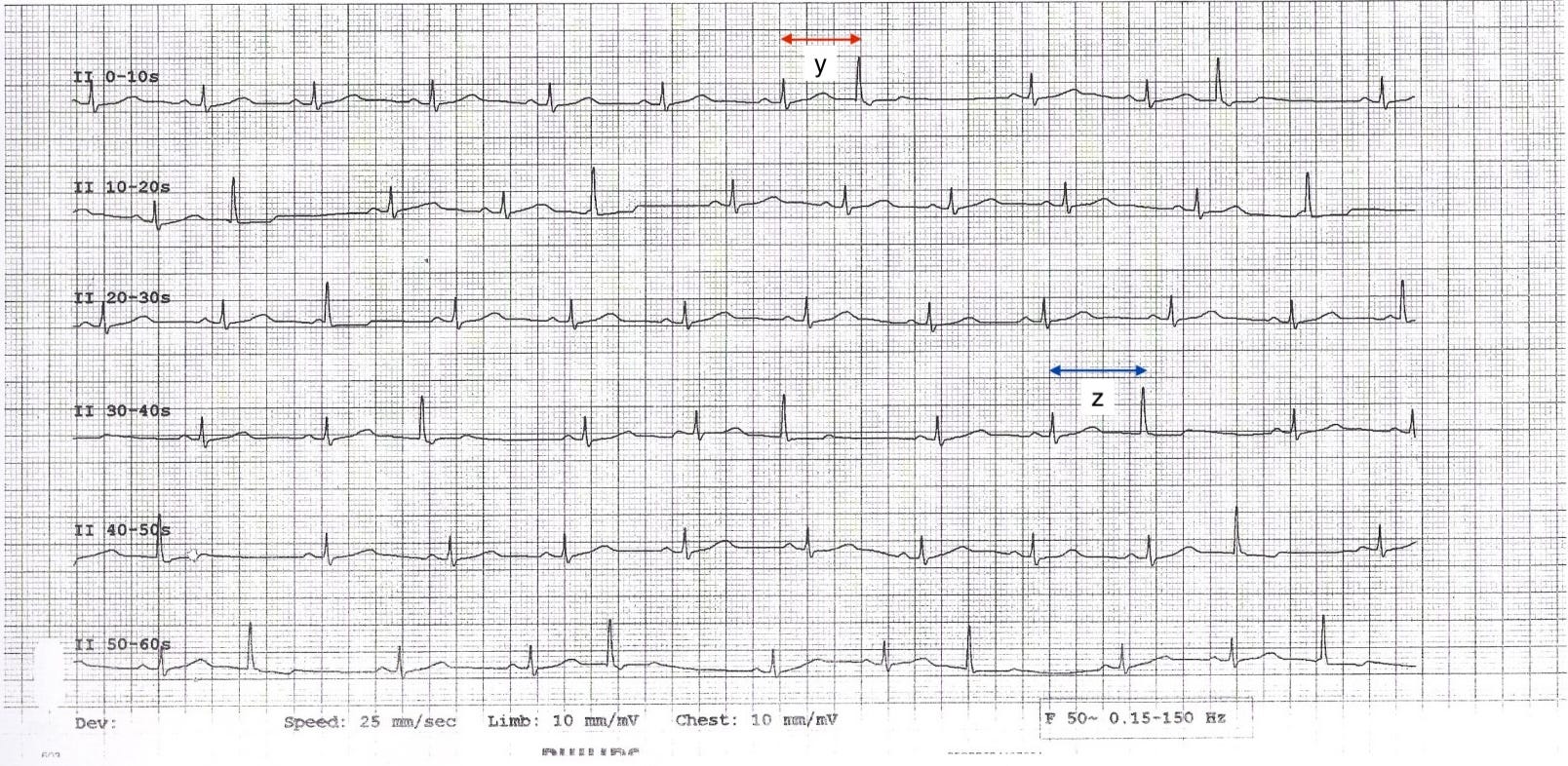
3. Fusion beats. Occasionally (not in this case), the sinus impulse and the ectopic impulse reach the ventricles at almost the same time, each depolarising part of the myocardium. The resulting QRS is a hybrid: narrower than a full ectopic beat but wider than a normal sinus beat. Fusion beats are not unique to parasystole; they also occur in ventricular tachycardia, paced rhythms, and pre-excitation.
What about the origin of these beats?
This goes beyond the question, but the morphology raises an interesting point.
Conventional teaching files this under “ventricular parasystole.” But the QRS duration of the ectopic beats is roughly 120 ms, possibly less — far narrower than the >160 ms expected from a typical ventricular myocardial ectopic, where the impulse conducts cell-to-cell. A narrower QRS suggests the impulse is using part of the conduction system, pointing toward a fascicular or Purkinje origin rather than ventricular myocardium. The detailed lead-by-lead morphology gives mixed signals about the exact location.1
From the question’s perspective, “parasystole” is the answer regardless of where the focus sits. The variable coupling intervals and interectopic intervals that are multiples of a common denominator are the diagnostic features.
Incorrect options
Premature atrial complexes. PACs are preceded by a premature P wave (often hidden in the T wave of the previous beat, distorting its shape). The ectopic beats here have no consistent preceding P wave. PACs also produce a narrow QRS unless they conduct aberrantly, and even aberrantly conducted PACs wouldn’t explain the variable coupling intervals or mathematically related interectopic intervals seen here.
Premature junctional complexes. PJCs originate at or near the AV node and typically produce a narrow QRS that resembles the sinus beat. They may have retrograde P waves (inverted in the inferior leads, appearing just before or after the QRS). The ectopic beats here are wider than the sinus beats, and the variable coupling intervals with mathematically related interectopic intervals point to parasystole rather than simple junctional ectopy.
Premature ventricular complexes. The most tempting answer. The ectopic beats are wider than sinus beats with no preceding P wave, which looks like PVCs. But “premature” implies a fixed temporal relationship to the preceding sinus beat, and that’s exactly what’s missing. Parasystolic beats fire on their own schedule, independent of sinus rhythm. Some land early (looking premature), others land later (looking more like escape beats). Their timing relative to the sinus cycle depends entirely on where two independent clocks happen to overlap. Parasystole is the more accurate answer because it identifies the mechanism, not just the morphology.
Junctional escape complexes. Escape beats are a passive mechanism: a lower pacemaker fires only when the sinus node fails to deliver a timely impulse, because it is normally suppressed by the sinus rhythm (overdrive suppression). In parasystole, the mechanism is active: the ectopic focus fires on its own schedule, protected by entrance block, regardless of what the sinus node is doing. Some parasystolic beats may land late enough in the cycle to resemble escape beats (the fifth complex on this ECG is an example), but the interectopic intervals that are multiples of a common denominator and the variable coupling intervals identify the rhythm as parasystole, not escape.
Is parasystole benign?
Parasystole is traditionally considered a benign electrophysiological phenomenon. However, recent evidence challenges this assumption. Do et al. (2023) studied 374 patients with ICDs and found parasystole in 9%, with a significantly higher rate of ventricular fibrillation compared to those without (36% vs 11%).2
Summary
How to identify parasystole on an ECG:
Ectopic beats with variable coupling intervals. The gap between the preceding sinus beat and the ectopic beat changes every time. This rules out standard PVCs (which have fixed coupling).
Interectopic intervals are multiples of a common denominator. The ectopic focus fires at a fixed cycle length. Visible intervals between ectopic beats are multiples of that base interval (1X, 2X, 3X), with “missing” beats explained by exit block.
Fusion beats. When sinus and ectopic impulses collide, the QRS is a hybrid of both morphologies (not seen in this ECG, though).
References
Do DH, O'Meara K, Lee J, Meyer S, Hanna P, Mori S, Fishbein MC, Boyle NG, Elizari MV, Bradfield JS, Shivkumar K. Ventricular Parasystole in Cardiomyopathy Patients: A Link Between His-Purkinje System Damage and Ventricular Fibrillation. JACC Clin Electrophysiol. 2023 Jul;9(7 Pt 1):936-948. doi: 10.1016/j.jacep.2022.11.014. Epub 2023 Feb 22. PMID: 37438043.
The limb leads show rS in aVL and qR in aVF (right axis deviation, LPFB-like pattern), suggesting a left anterior fascicular origin. But V1 shows rS (LBBB-like, predominantly negative), which is more consistent with a right-sided origin — left fascicular ectopy classically produces RBBB morphology in V1. V5–V6 show Rs with S waves, which doesn't match clean LBBB or typical junctional aberrancy. A septal origin near the Purkinje network could reconcile the LBBB-like V1 with right axis deviation, but the exact origin remains uncertain.
Parasystolic foci in this cohort were predominantly from the His-Purkinje system.

Indeed a step by step explanation on how parasystole works! Thanks a lot Ioannis!