QRS complex
Duration, voltage, axis, and morphology: a systematic guide to reading the QRS complex on a 12-lead ECG.
The QRS complex is the largest deflection on the ECG. It begins at the first departure from baseline after the PR segment and ends where the tracing returns to baseline at the J point. It is called a “complex” because it combines two or three individual waves rather than a single deflection.
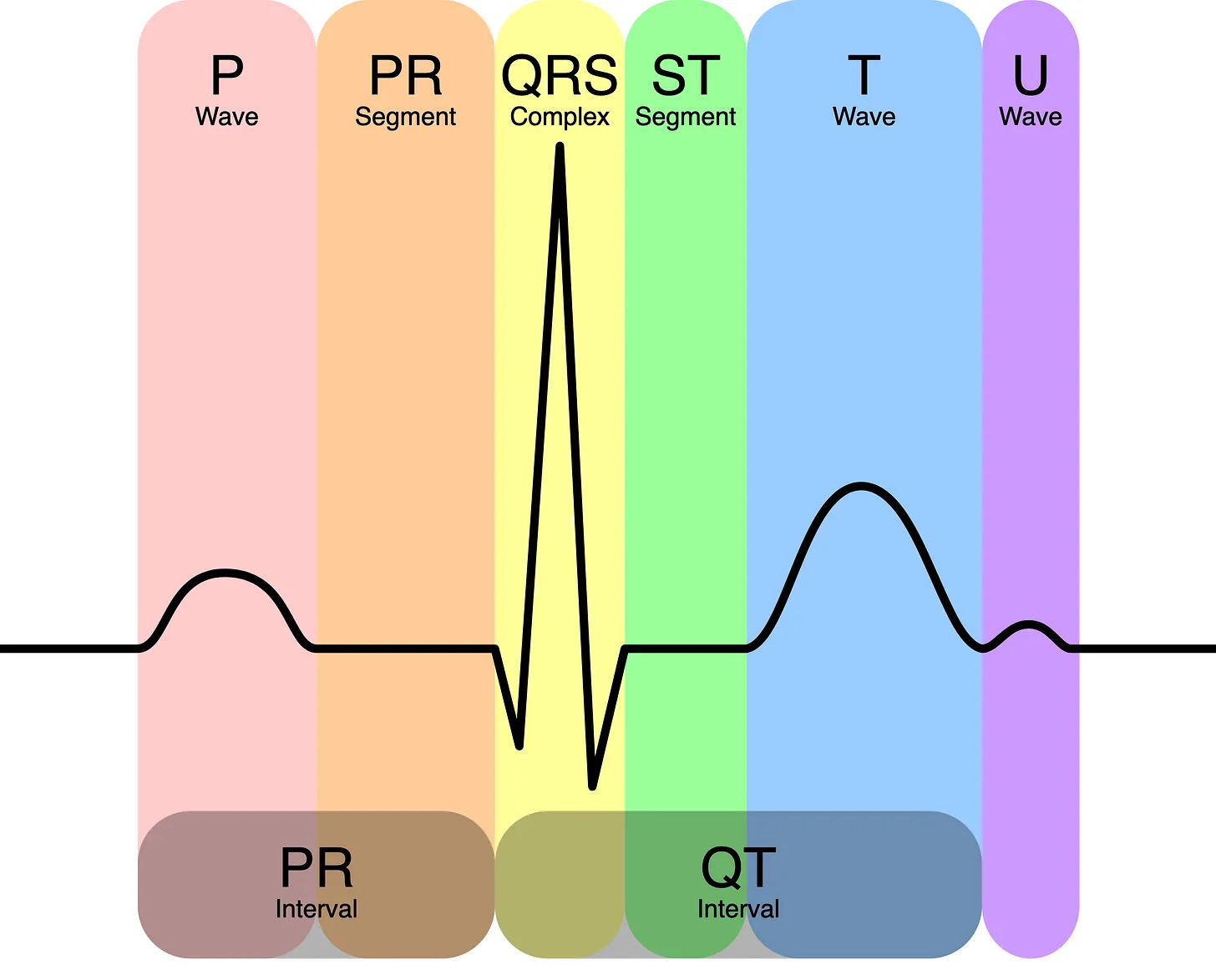
Four parameters are assessed: duration, voltage, axis, and morphology.
Physiological representation
The QRS complex represents ventricular depolarisation [1].
After passing through the AV node, the impulse enters the bundle of His, which splits into the left and right bundle branches. The left bundle branch further divides into an anterior fascicle and a posterior fascicle. Both bundle branches ramify into the Purkinje fibre network, a dense web of specialised conducting fibres that delivers the impulse rapidly across the ventricular endocardium. Depolarisation then spreads from endocardium to epicardium through the ventricular wall.
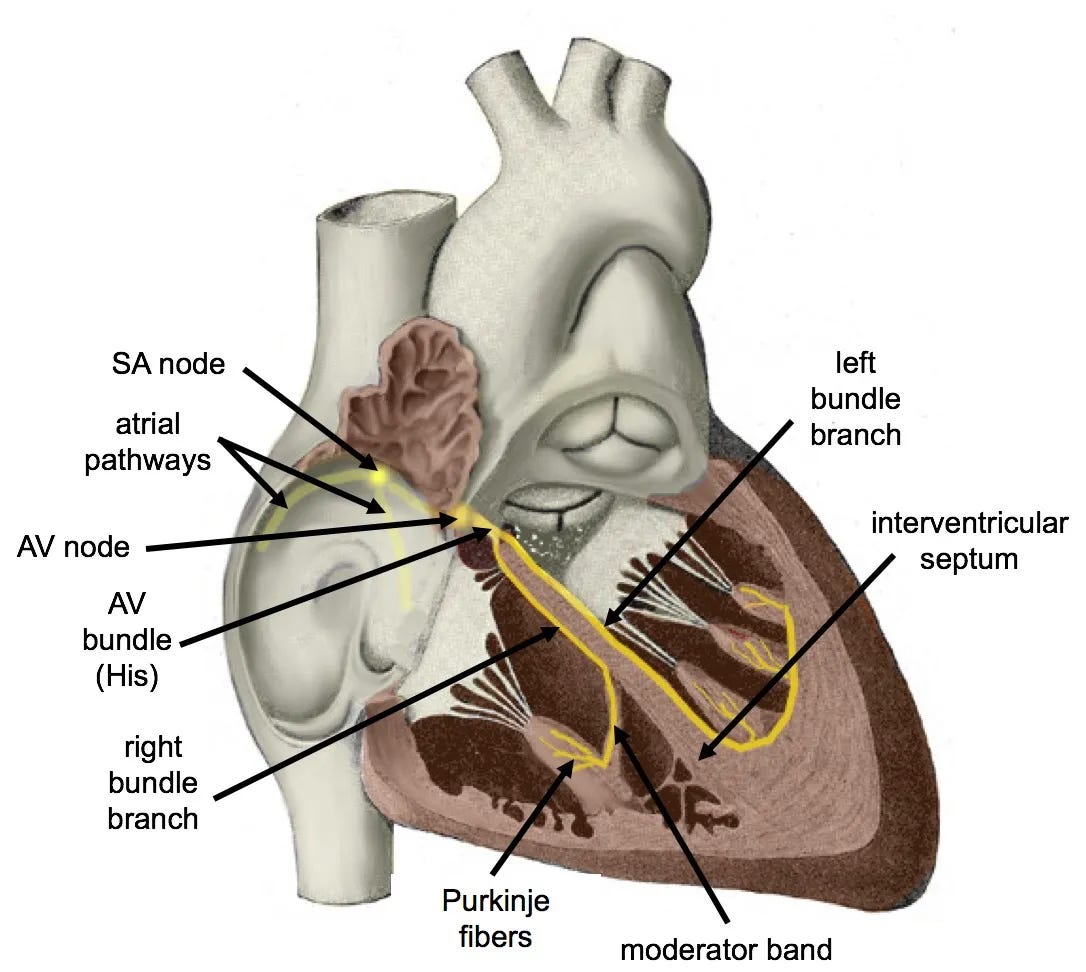
Normal ventricular depolarisation occurs in three phases. Understanding these phases explains why the QRS looks the way it does in V1 and V6.
V1 and V6 are used here because they sit at opposite ends of the precordial leads: V1 is the only lead positioned over the right ventricle, V6 overlies the left. Because the bundle branches split the conduction system into right and left pathways, these two leads capture the depolarisation sequence from directly opposing viewpoints.
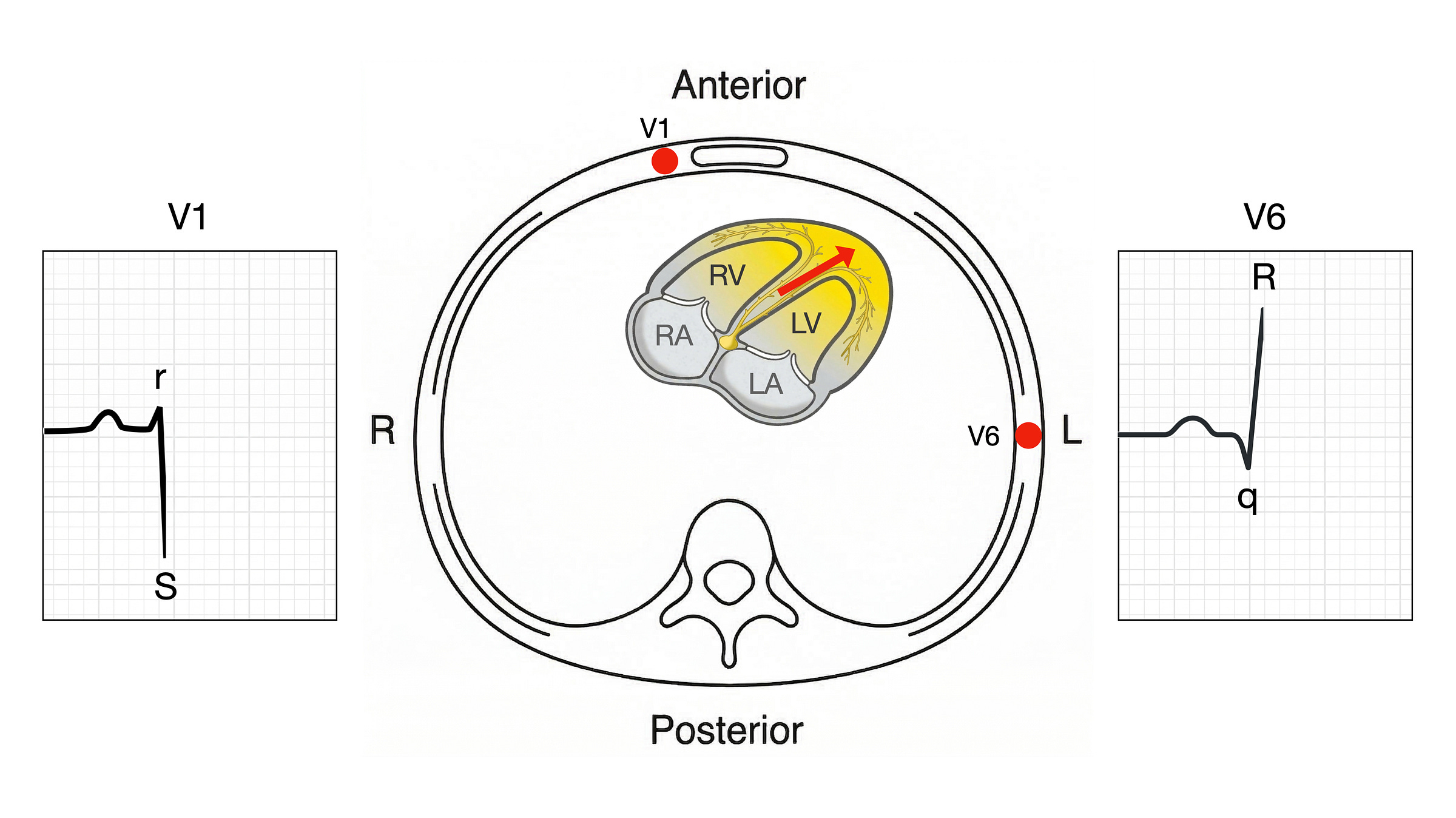
Phase 1: septal depolarisation
The interventricular septum depolarises first, from left to right. The left bundle branch activates the left side of the septum slightly before the right bundle branch activates the right side [1].
This produces a depolarisation vector pointing from left to right across the chest. V1 sits on the anterior chest wall, close to the right ventricle. V6 sits on the left lateral chest wall, over the left ventricle. A vector moving towards an electrode produces a positive deflection; a vector moving away produces a negative deflection.
The left-to-right septal vector points towards V1, producing a small positive deflection: the r wave. It points away from V6, producing a small negative deflection: the q wave. By convention, small deflections are written in lowercase (r, q, s) and large ones in uppercase (R, S). Both deflections are small because the septum is a thin structure with relatively little muscle mass.
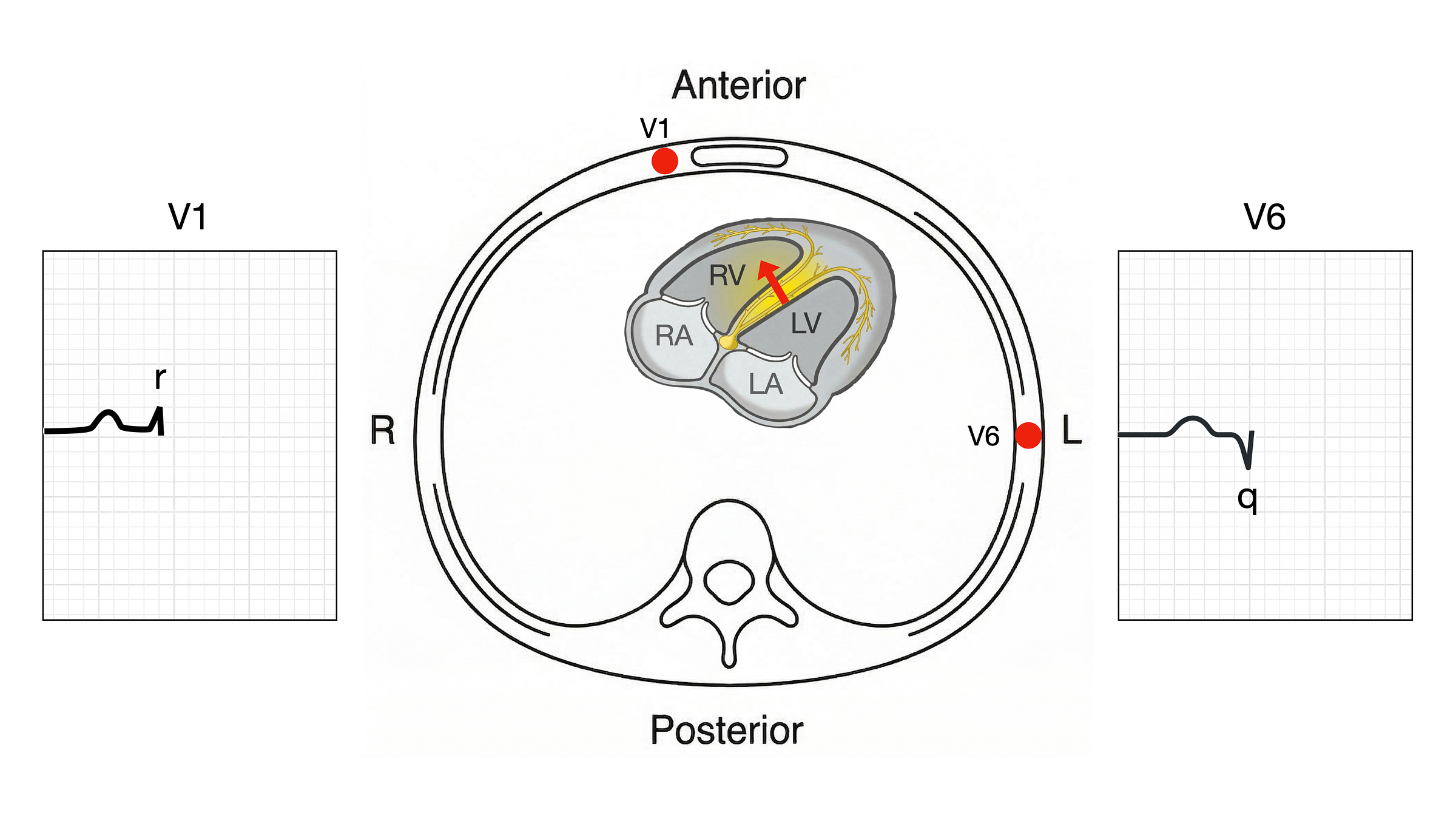
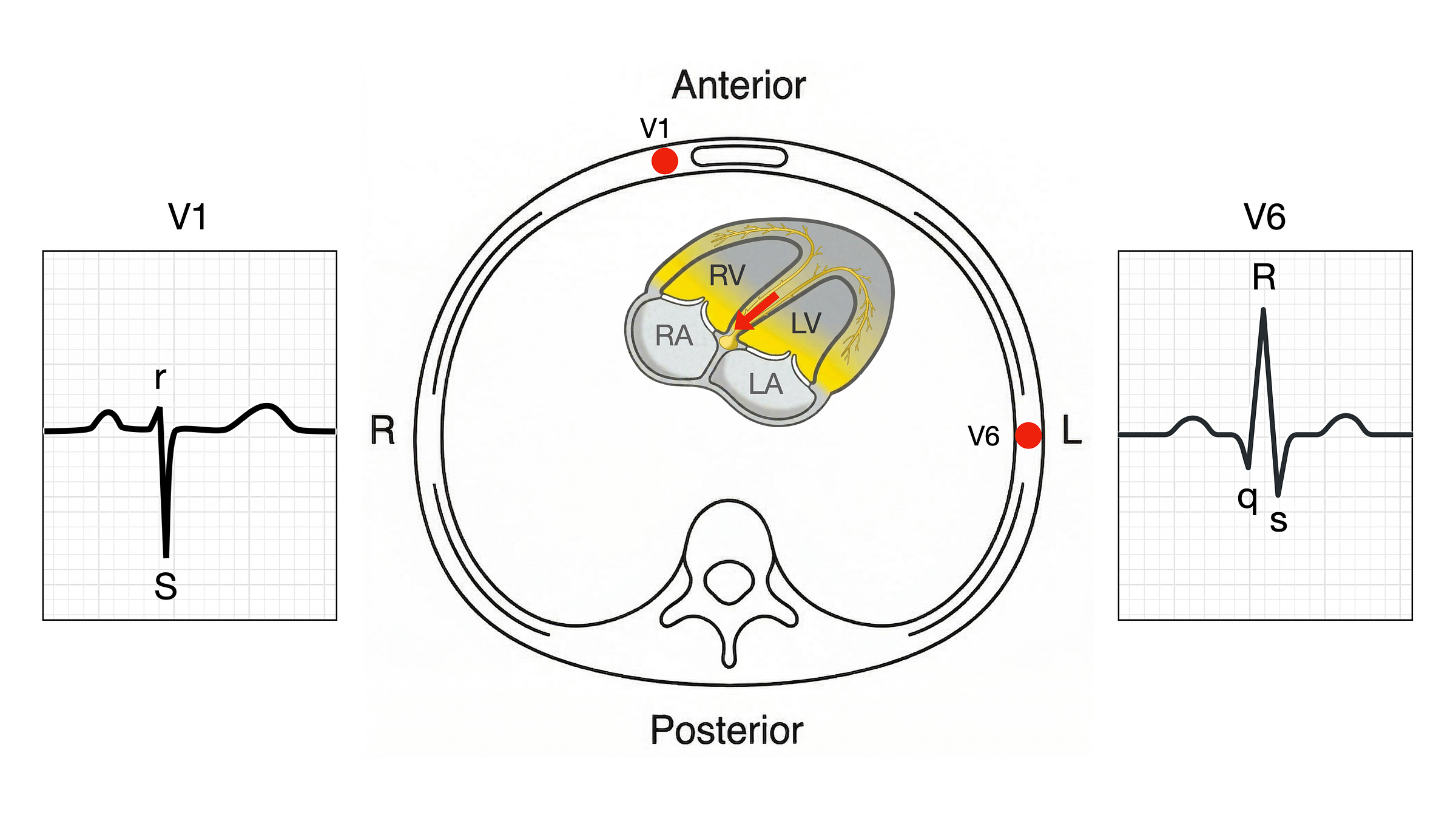
Phase 2: free wall depolarisation
Both ventricular free walls depolarise simultaneously, as electrical impulses travel to the ventricles from both bundle branches. However, the left ventricle has far greater muscle mass than the right, so the leftward electrical forces dominate. The resultant depolarisation vector points to the left, towards V6 and away from V1 [1].
This vector points away from V1, producing a deep negative deflection: the S wave. It points towards V6, producing a tall positive deflection: the R wave. Both deflections are large because the ventricular free walls contain much more muscle mass than the septum.
Phase 3: terminal depolarisation
The basal and posterior walls are the last regions to depolarise. The terminal depolarisation vector points posteriorly and to the right, away from V6.
This vector is directed almost perpendicular to V1, so it has little effect on V1, which retains its rS pattern. In V6, it adds a small negative deflection after the R wave: a terminal s wave.
The result: rS in V1, qRs in V6
Combining the three phases: V1 records a small r (septal, towards) followed by a deep S (free wall, away), giving an rS pattern. The terminal vector is nearly perpendicular to V1 and has little effect on it. V6 records a small q (septal, away), a tall R (free wall, towards), and a small s (terminal posterior, away), giving a qRs pattern. The terminal s wave is often subtle, which is why V6 is commonly described simply as qR. This morphology follows entirely from the anatomy.
Duration
Normal QRS duration is less than 120 ms (less than 3 small squares) [1].
The QRS is narrow because the Purkinje system activates both ventricles almost simultaneously. It widens when part or all of the ventricular myocardium is depolarised without the Purkinje system, or when conduction itself is slowed.
Four mechanisms of wide QRS:
The Purkinje system is partially blocked (i.e. bundle branch block). One bundle branch fails, so that ventricle depolarises via slow myocyte-to-myocyte conduction across the septum. The other ventricle activates normally. This is an intraventricular conduction delay1.
The Purkinje system is bypassed entirely. The impulse either originates in ventricular myocardium (ventricular ectopics, idioventricular rhythm) or is delivered directly to it (paced rhythm). In both cases, depolarisation spreads cell-to-cell at ~0.5 m/s instead of 4 m/s.
The ventricle is pre-excited (WPW). An accessory pathway delivers the impulse to ventricular myocardium before the normal impulse arrives via the AV node. The early part of depolarisation travels slowly through myocardium, producing a delta wave. The rest of the ventricle is activated normally via the Purkinje system.
Conduction velocity is globally slowed (hyperkalaemia). Elevated potassium slows conduction through all tissue, progressively widening the QRS.
Voltage
Normal QRS voltage means no ventricular hypertrophy criteria are met (not too large), and the complexes are not abnormally small (not too small).
High voltage: left ventricular hypertrophy
LVH increases the muscle mass generating the QRS, which amplifies voltage in the leads overlying the left ventricle.
Two commonly used criteria:
Sokolow-Lyon: S-wave depth in V1 + R-wave height in V5 or V6 >= 35 mm
Cornell: R-wave height in aVL + S-wave depth in V3 > 28 mm (men) or > 20 mm (women)
Voltage criteria alone have low sensitivity for LVH. When combined with a strain pattern (ST depression and T-wave inversion in the lateral leads), specificity improves considerably.
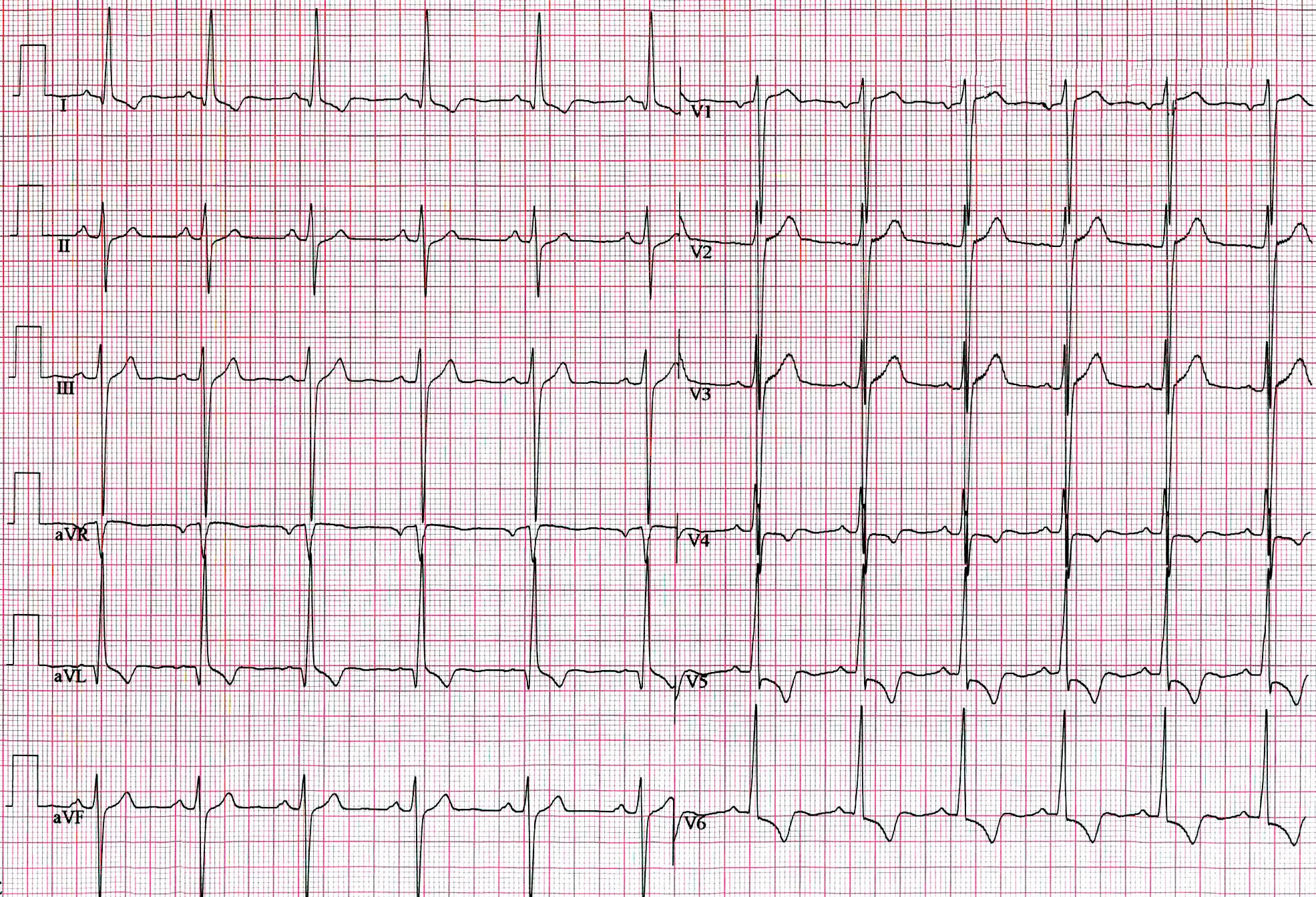
High voltage: right ventricular hypertrophy
RVH is suggested by a dominant R wave in V1 (R:S ratio > 1) with right axis deviation. Normally, the left ventricle dominates and V1 shows a small r wave followed by a deep S wave. When the right ventricle hypertrophies, its contribution to the QRS grows, eventually producing a tall R wave in V1.
A tall R wave in V1 has a differential diagnosis beyond RVH:
Posterior MI (loss of posterior forces makes the anterior R appear dominant)
RBBB (the R’ in V1 can mimic a dominant R)
WPW type A (pre-excitation via a left-sided accessory pathway)
Low voltage
Low QRS voltage is defined as:
less than 5 mm peak-to-trough in all limb leads, or
less than 10 mm in all precordial leads.
The key word is “all”: a single low-amplitude lead does not qualify.
Causes fall into two categories:
Impaired voltage generation: the ventricular myocardium itself is diseased (e.g. cardiomyopathy, MI, amyloidosis)
Increased impedance: something between the heart and electrodes attenuates the signal, whether air (COPD), fluid (pericardial effusion), or electrically inert tissue (fat)
Electrical alternans
Electrical alternans describes QRS voltage alternating beat-to-beat, typically between higher and lower amplitudes in a regular pattern. It is highly specific for cardiac tamponade, where a large pericardial effusion causes the heart to physically swing back and forth within the fluid-filled sac. Each swing changes the heart’s position relative to the chest electrodes, producing alternating QRS amplitudes. Sensitivity is low (present in a minority of tamponade cases), but when present it should prompt urgent echocardiographic assessment.
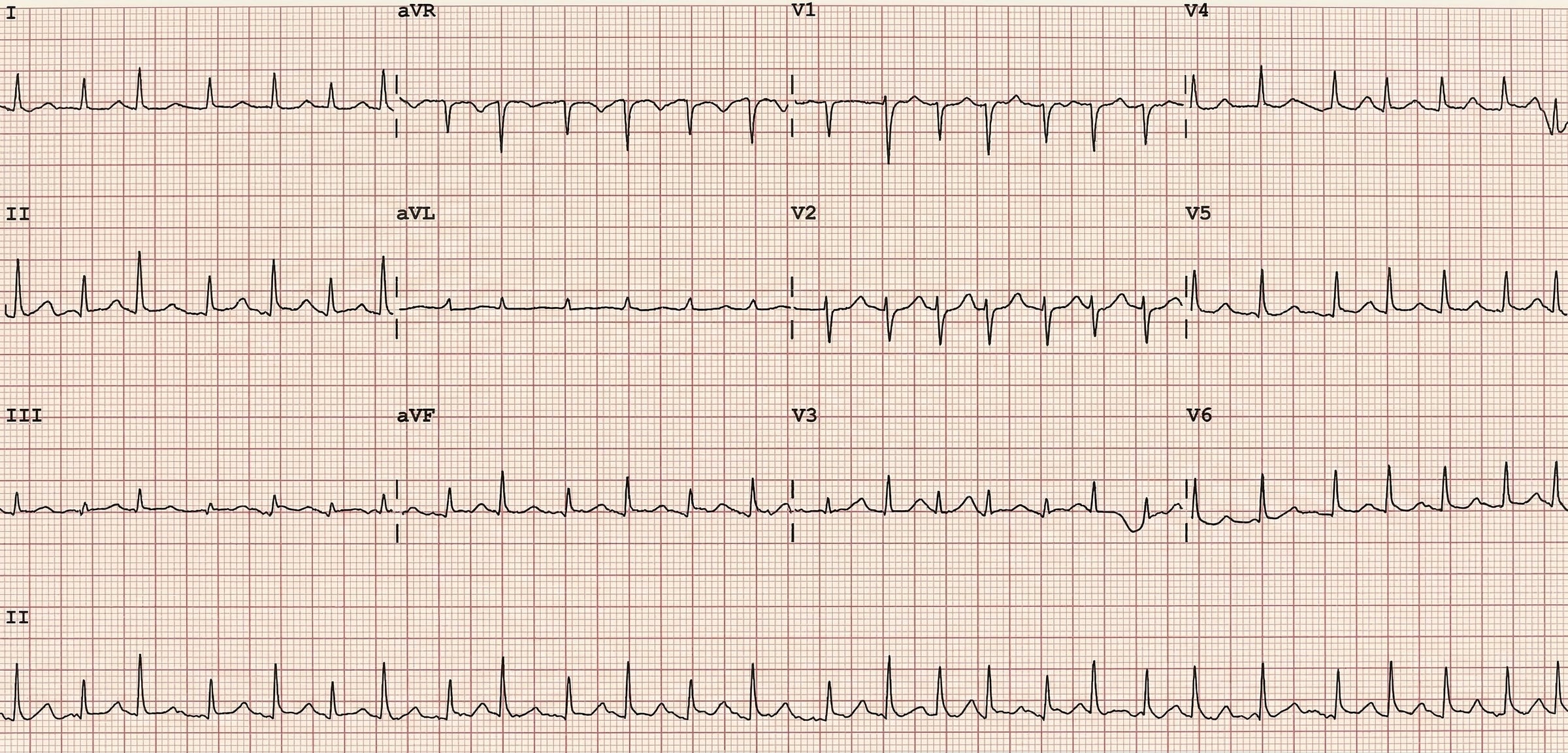
Axis
The normal QRS axis is -30 to +90 degrees [1]. A quick check: if the QRS is positive in both lead I and lead II, the axis is normal.
Left axis deviation (LAD): more negative than -30 degrees. Common causes: LAFB, LVH, inferior MI.
Right axis deviation (RAD): more positive than +90 degrees. Common causes: RVH, LPFB, PE, lateral MI.
Extreme axis deviation: between -90 and +/-180 degrees. Common causes: severe hyperkalaemia, VT, severe RVH.
Further reading: How to find the QRS axis in under 3 seconds
Morphology
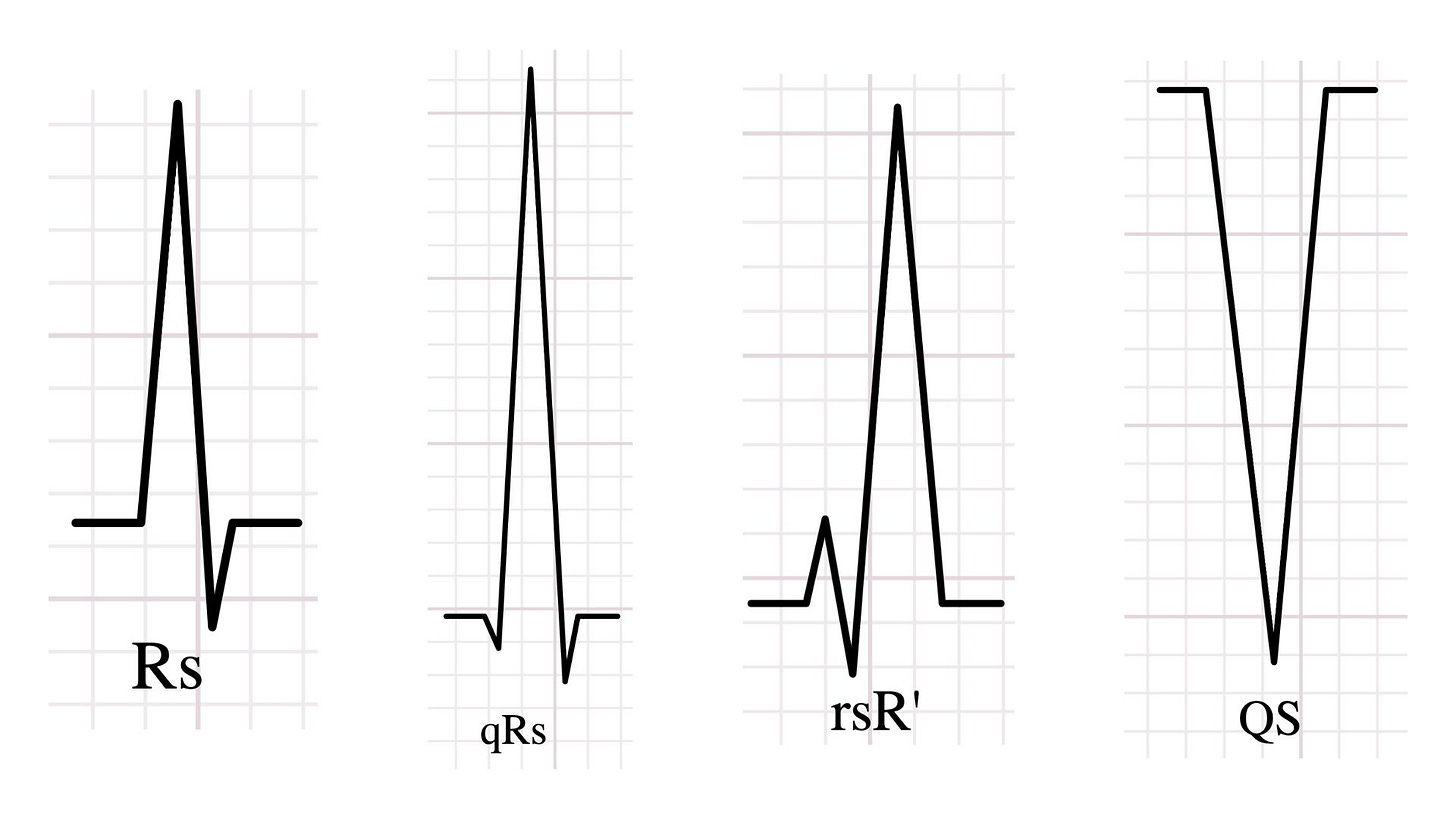
QRS nomenclature
The QRS nomenclature is the language used to describe QRS morphology. The naming rules are straightforward:
Q wave: the first negative deflection
R wave: the first positive deflection
S wave: a negative deflection following the R wave
R’ wave: a second positive deflection (after S)
QS complex: an entirely negative complex with no positive deflection
Uppercase letters (Q, R, S) denote waves taller or deeper than 5 mm (0.5 mV). Lowercase letters (q, r, s) denote waves smaller than 5 mm.
Normal QRS morphology
The normal QRS morphology follows directly from the three phases described above. Across the precordial leads, the QRS transitions from an rS pattern in V1 to a qR pattern in V6. Each intermediate lead captures a progressively more LV-dominant vector. The transition zone, where the R wave first becomes taller than the S wave, normally occurs around V3-V4. This gradual increase in R-wave amplitude from V1 to V6 is called R-wave progression.
The small q waves seen in the lateral leads (I, aVL, V5-V6) reflect normal left-to-right septal depolarisation and should not be confused with pathological Q waves.
Abnormal QRS morphology
Pathological Q waves: indicate electrically silent scar, most commonly prior MI [2].
Delta wave: slurred QRS upstroke from ventricular pre-excitation (WPW).
RBBB pattern: rsR’ in V1-V2, broad S wave in I and V6.
LBBB pattern: broad, notched R in I and V5-V6, QS or rS in V1-V2.
Poor R-wave progression: R wave fails to become dominant by V3-V4. Consider lead misplacement first.
Fragmented QRS (fQRS): additional R waves or notching indicating myocardial scarring [3].
Further reading: QRS complex nomenclature and morphology
Summary
The QRS complex represents ventricular depolarisation.
It is assessed by four parameters:
duration (normal < 120 ms, wide QRS when the Purkinje system is blocked, bypassed, pre-excited, or globally slowed)
voltage (high voltage suggests ventricular hypertrophy, low voltage suggests impaired generation or increased impedance)
axis (normal -30 to +90 degrees)
morphology (normal rS in V1 transitioning to qR in V6)
References
Lilly LS. Pathophysiology of Heart Disease. 7th ed. Wolters Kluwer; 2021.
Thygesen K et al. Fourth Universal Definition of Myocardial Infarction (2018). Eur Heart J. 2019;40(3):237-269.
Take Y, Morita H. Fragmented QRS: What Is The Meaning? Indian Pacing Electrophysiol J. 2012;12(5):213-225.
Fascicular blocks (LAFB, LPFB) may mildly prolong the QRS (100-120 ms) but cause axis deviation rather than true widening, so they do not meet the 120 ms threshold.