"A rhythm issue" | ECG challenge #8
A 28-year-old with recurrent palpitations presents with a fast, irregular, wide-complex tachycardia. What does the ECG show?
A 28-year-old woman is brought to the emergency department by ambulance. She is pale, diaphoretic, and struggling to speak in full sentences. Her partner says she collapsed at home after complaining of palpitations. She has had episodes of fast heartbeats since her teens. She was seen for a “rhythm issue” in her home country but has no records and no specific diagnosis available at this time.
She has no other medical history and takes no regular medication.
On examination, her heart rate is approximately 180 bpm and irregular. Blood pressure is 80/50 mmHg. GCS 14 (E3 V5 M6).
An ECG is performed.
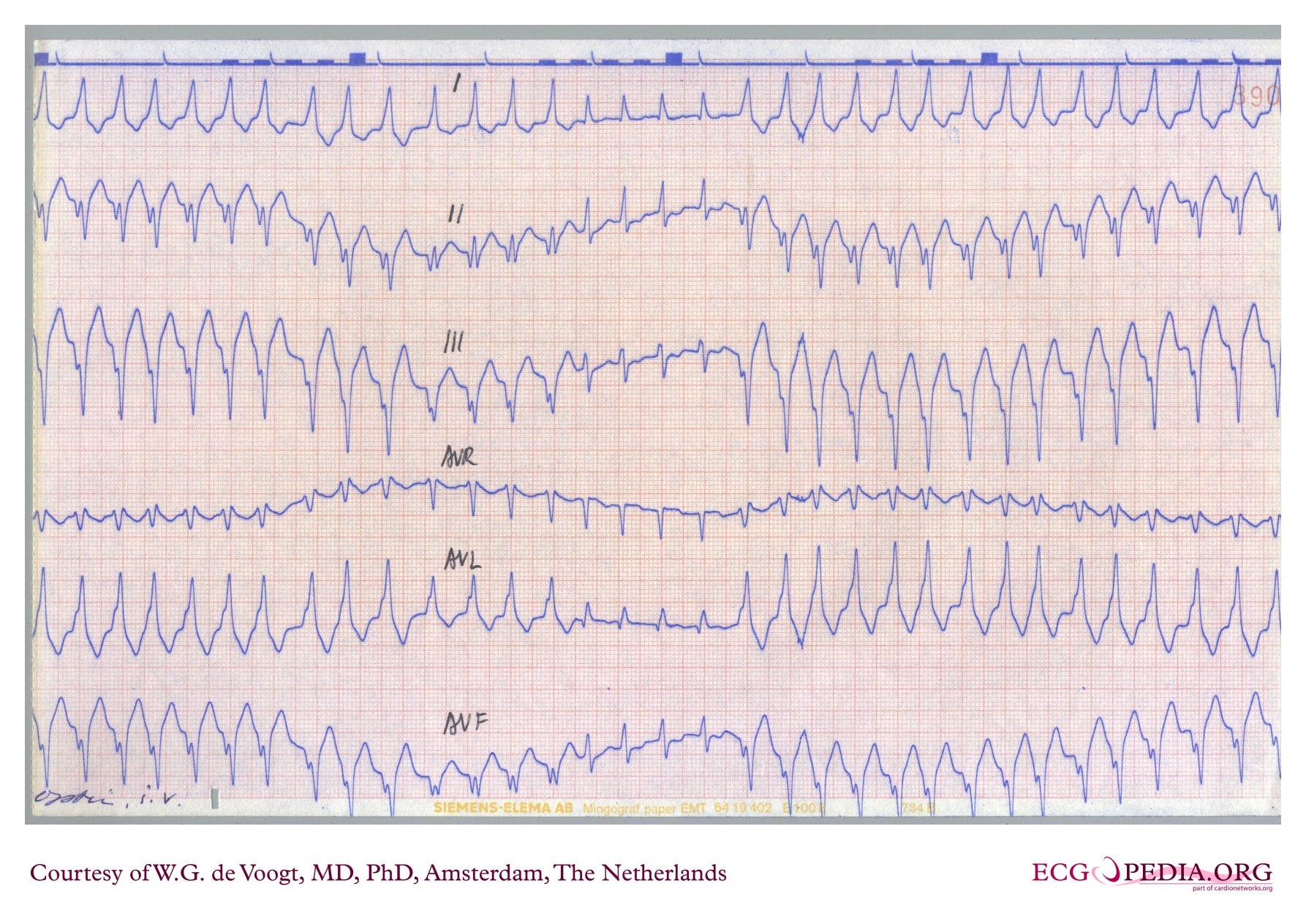
ECG systematic analysis
Assumed paper speed: 25 mm/s and voltage: 10 mm/mV (standard).
This ECG shows limb leads only (I, II, III, aVR, aVL, aVF), presented as rhythm strips stacked vertically.
Rhythm: Irregularly irregular.
P waves: Absent. No discernible P waves in any lead.
PR interval: Not applicable (no organised atrial activity).
QRS complex:
Rate: ~180 bpm.
Duration: ~120 ms, widened by delta waves.
Axis: Variable. Lead I remains positive throughout. Lead II shifts from negative (left axis deviation) to positive (normal axis) and back, correlating with changes in QRS morphology.
Morphology: Varies throughout the recording. Most beats show wide QRS complexes with delta waves (a slurred initial deflection of the QRS), consistent with ventricular pre-excitation. The delta waves are positive in some leads and negative in others (clearly visible as negative deflections in lead II). The middle portion of the strip shows beats with slightly narrower QRS complexes and a normalised axis, consistent with fusion beats.
Voltage: Normal.
QT interval: Not reliably measurable at this rate with pre-excitation.
ST segment: Not reliably assessable due to wide QRS and rapid rate.
T waves: T-wave inversion in I and aVL (apart from the middle portion of the strip).
Overall, an irregularly irregular tachycardia at ~180 bpm with wide QRS complexes showing delta waves and variation in QRS morphology and axis. The combination of absent P waves, irregular rhythm, pre-excitation, and varying morphology is consistent with atrial fibrillation with ventricular pre-excitation via an accessory pathway (pre-excited AF).
Correct answer
Atrial fibrillation with pre-excitation (pre-excited AF).
This ECG might look like ventricular tachycardia at first glance. Wide QRS complexes, fast rate, haemodynamically compromised patient. But the rhythm is irregularly irregular. Monomorphic VT is regular. Polymorphic VT can be irregular with varying morphology, but it does not produce delta waves. On this ECG, the QRS complexes show delta waves and the morphology varies between fully pre-excited beats and fusion beats. That pattern points to two competing conduction routes (AV node and accessory pathway), not a ventricular origin.
What you’re looking at is atrial fibrillation conducted through an accessory pathway: a strip of conducting tissue that bridges the atria and ventricles outside the normal conduction system [1]. Every ECG feature on this strip follows from one fact: in AF, chaotic atrial impulses can reach the ventricles via two routes simultaneously, the AV node and the accessory pathway, and the balance between them shifts continuously.
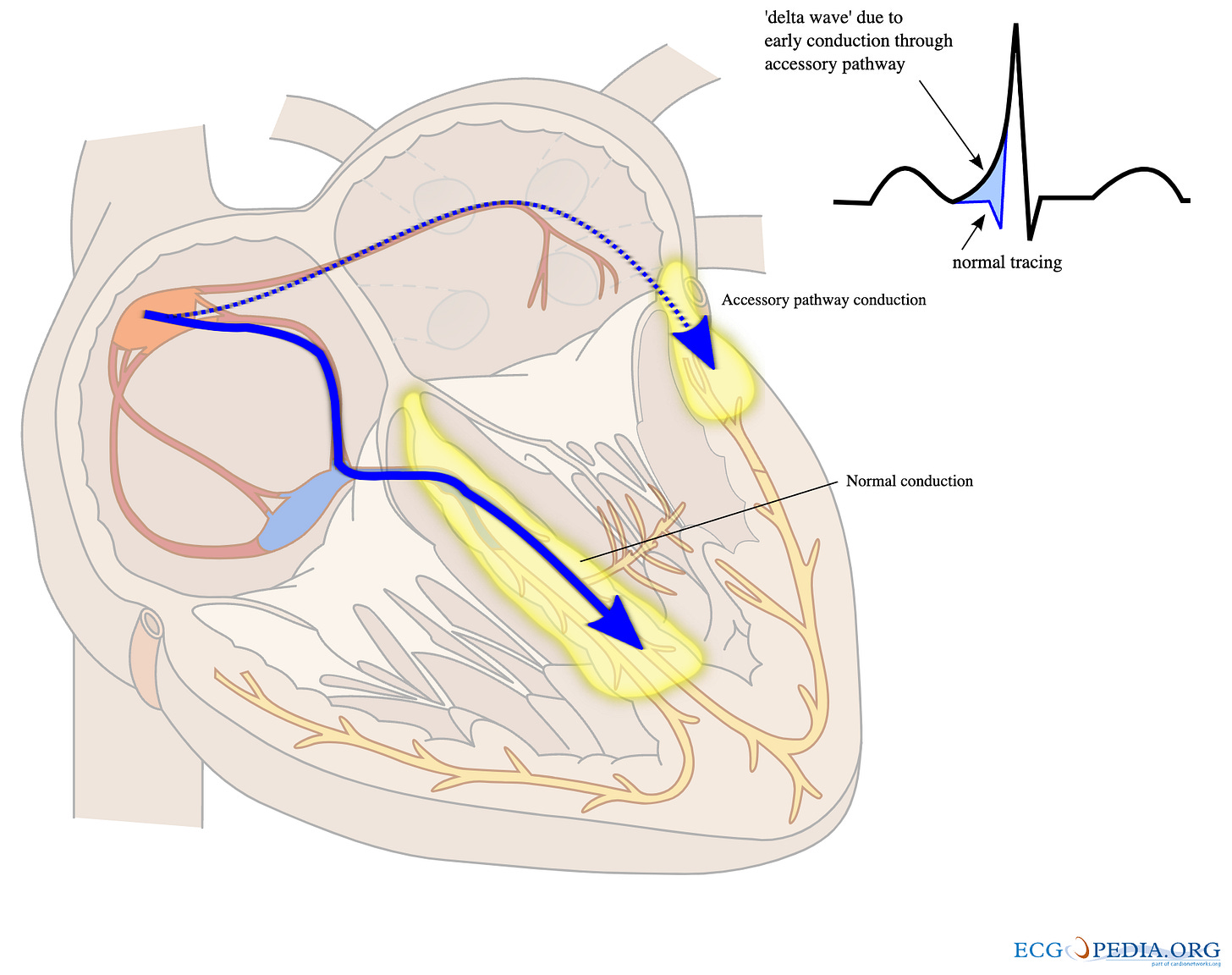
Wide QRS with delta waves. When the accessory pathway activates most of the ventricle, depolarisation starts at the pathway’s insertion point and spreads through the myocardium cell-to-cell, bypassing the His-Purkinje system. This produces a wide QRS with a delta wave: a slurred initial deflection at the start of the QRS. The delta wave can be positive or negative depending on the lead and the direction of the initial depolarisation vector relative to that lead. On this ECG, the delta waves are negative in lead II (the vector is directed away from lead II, superiorly) and positive in other leads.
Varying QRS morphology. Each beat’s QRS depends on which route gets there first and how much of a head start it has. Fully pre-excited beats (accessory pathway dominates) are wide with prominent delta waves. Fusion beats1 are slightly narrower, with less prominent delta waves.
Axis shifts. The electrical axis follows the morphology. Fully pre-excited beats show left axis deviation (negative delta waves in lead II indicate the initial vector is directed superiorly). Fusion beats show a more normalised axis (lead II becomes less negative or positive) as the AV node contributes more to ventricular activation. This is visible in the middle portion of the strip.
Fast ventricular rate. The AV node has a long refractory period that limits how many impulses reach the ventricles. The accessory pathway often does not have this limitation. It can conduct atrial impulses at rates the AV node would never allow [1][2].
Irregularly irregular rhythm. The underlying rhythm is atrial fibrillation. Chaotic atrial impulses arrive at both pathways at random intervals.
Incorrect options
Monomorphic VT. The most important differential. Monomorphic VT produces wide QRS complexes at a fast rate, but it is typically regular (or nearly so) with a fixed QRS morphology and a constant axis.
Polymorphic VT. Polymorphic VT does show varying QRS morphology and can be irregular, making it an important differential. The key distinction: pre-excited AF shows delta waves consistent with an accessory pathway.
Atrial fibrillation with aberrant conduction. AF with aberrant conduction (e.g. rate-related bundle branch block) produces wide QRS complexes, but the widening is due to conduction delay in the His-Purkinje system, not pre-excitation. The wide beats most commonly show an RBBB pattern (the right bundle branch has the longest refractory period), not delta waves. In Ashman phenomenon, wide complexes appear intermittently following a long-short RR sequence and revert to narrow QRS [3].
Atrial flutter with variable block. Flutter with variable block produces an irregular ventricular rate, but sawtooth flutter waves should be visible, particularly in the inferior leads. No flutter waves are seen here. Flutter also does not explain the delta waves or varying QRS morphology.
Why is pre-excited AF an emergency?
Pre-excited AF is dangerous because the accessory pathway can conduct atrial impulses at rates the AV node would never allow [1][2]. In ordinary AF, the AV node’s long refractory period acts as a gatekeeper, limiting how many impulses reach the ventricles. The accessory pathway may not have this limitation. If it has a short refractory period, it can conduct at very high rates, producing ventricular rates that are haemodynamically intolerable. Pre-excited AF can degenerate into ventricular fibrillation [1][2].
At this ventricular rate, the patient is likely haemodynamically unstable. Follow your ALS algorithm: if adverse features are present, synchronised electrical cardioversion and seek expert help [1][2].
On top of that, the wrong drug can make things worse. In pre-excited AF, the AV node is protective. Every impulse that conducts through the AV node depolarises the ventricles and leaves the myocardium in a refractory state before the accessory pathway can activate it. The AV node is effectively competing with the accessory pathway, limiting how fast the ventricles can be driven. Block the AV node and you remove that protection, allowing the accessory pathway to drive the ventricles unopposed at even faster rates.
Adenosine is a characteristic drug to avoid, precisely because of its potent AV nodal blockade.
Summary
How to identify pre-excited AF on an ECG:
Irregularly irregular rhythm (atrial fibrillation).
Wide QRS complexes with delta waves (ventricular pre-excitation via an accessory pathway).
Variation in QRS morphology and axis (fully pre-excited and fusion beats), with delta waves present. Delta waves distinguish pre-excited AF from monomorphic VT (fixed morphology, no delta waves) and polymorphic VT (no delta waves).
Fast ventricular rate (the accessory pathway lacks the rate-limiting refractory period of the AV node).
Avoid AV nodal blocking agents (e.g. adenosine). Blocking the AV node removes its protective competition with the accessory pathway, increasing the ventricular rate and risking degeneration into ventricular fibrillation.
This is my interpretation of this ECG. If you see it differently or have another diagnosis in mind, let me know in the comments. I'm always happy to be corrected.
The accessory pathway behind pre-excited AF is the same one that produces AVRT, one of the (at least) four arrhythmias behind “SVT.” For more on how accessory pathways fit into the broader SVT picture, see the following article:
References
Brugada J, Katritsis DG, Arbelo E, et al. 2019 ESC Guidelines for the management of patients with supraventricular tachycardia. European Heart Journal. 2020;41(5):655-720.
Page RL, Joglar JA, Caldwell MA, et al. 2015 ACC/AHA/HRS Guideline for the Management of Adult Patients With Supraventricular Tachycardia: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. Circulation. 2016;133(14):e471-e505. doi:10.1161/CIR.0000000000000310
Grigg WS, Pearlman JD, Nagalli S. Ashman Phenomenon. [Updated 2024 Sep 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562311/
Fusion beats in pre-excited AF occur when an atrial impulse reaches the ventricles through both the accessory pathway and the AV node at nearly the same time. The accessory pathway depolarises part of the ventricle from its insertion point (producing a delta wave), while the AV node depolarises the rest via the His-Purkinje system (producing a normal QRS component). The resulting QRS is a hybrid: wider than a normally conducted beat (because of the pre-excited component) but narrower than a fully pre-excited beat (because the His-Purkinje system handles part of the activation).