Why Do YOU Learn ECG Interpretation?
Elon Musk, Learning, and the Real-World Importance of ECG Interpretation

Why even bother?
Why bother learning ECG interpretation? Sooner or later, AI will most likely do it for us. Why bother learning anything?
It’s NOT a rhetorical question!
Knowing why you do something allows you to be intentional about it. Pursue it wholeheartedly or abandon it.
Why I couldn’t learn ECG interpretation in the beginning
The reason is simple: I didn’t know why I wanted to learn. And I didn’t know why because I hadn’t encountered real-life problems. Learning ECGs hadn’t become relevant to me yet.
So I needed a problem to learn. The best place to find it was the hospital.

The patient who was having “seizures”
It was a tranquil evening during my fifth year of medical school. The hushed corridors of the tertiary hospital adjacent to my university echoed with the distant sounds of medical equipment. I found myself shadowing the on-call cardiology registrar (or resident).
While settled in an office outside the coronary care unit, we were discussing problems that you encounter in cardiology. (While these discussions are insightful, given the registrar's hands-on experience, they still felt somewhat abstract. After all, I was already drowning in hypothetical problems given by my medical school.)
Our conversation was interrupted by a knock. The door opened to reveal a slightly flustered vascular surgery registrar. He began describing a patient under his care who exhibited symptoms akin to "generalised seizures." The patient would lose consciousness momentarily, accompanied by sporadic twitching of his upper limbs and head.
I was puzzled. Why consult cardiology for what seemed like a neurological issue? Why not approach the neurology department?
Curiosity piqued, we made our way to the vascular ward. There, we met the patient: alert, coherent, and awaiting a toe amputation due to peripheral artery disease (PAD). He had all the risk factors of PAD and coronary artery disease (CAD), from diabetes mellitus to smoking. His wife sat beside him and recounted the events precisely as the vascular surgery registrar had earlier.
But then, without warning, the patient went into one of his episodes. His head tilted back, eyes rolled upwards, and his limbs began to twitch. The cardiology registrar swiftly checked the patient's radial pulse. "He has no pulse!" he declared. A crash call was sounded, but before the medical team could fully respond, the patient regained consciousness, appearing as if nothing had happened.
His ECG (when back to normal and alert) looked like the following one:
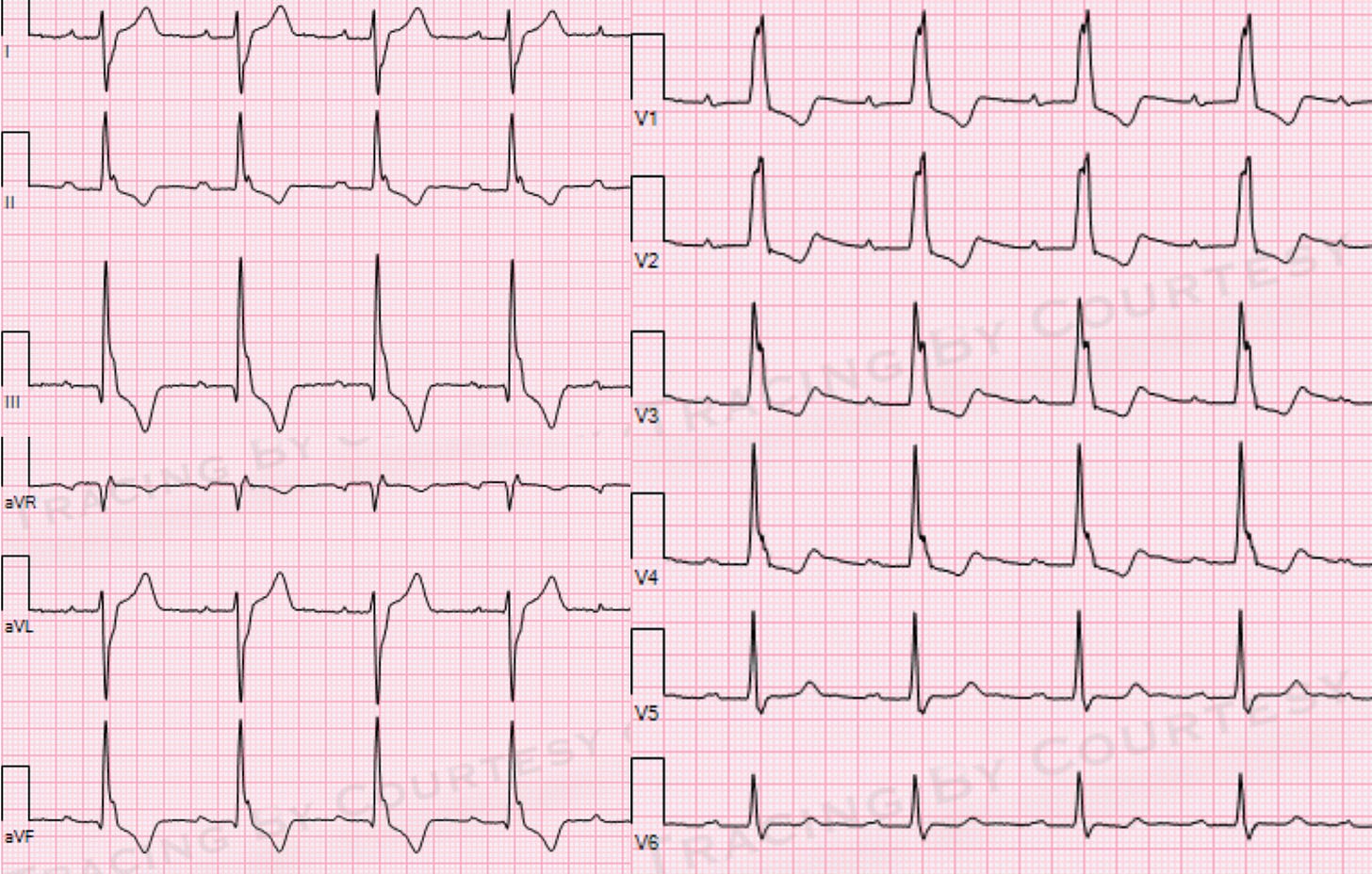
This ECG, mirroring our patient's, indicates three blocks: two intraventricular and one atrioventricular (AV) block:
RBBB (intraventricular) (read this post for bundle branch blocks)
LPFB (read this post for left fascicular blocks)
1st-degree AV block
This is traditionally known as trifascicular block. This term, however, is nowadays deemed inaccurate as the conduction delay resulting in the PR interval prolongation does not usually occur in a fascicle but in the AV node¹.
The risk with this block is that it can lead to a higher degree AV block, like 2nd-degree Mobitz II or even a complete AV block. If it goes into a complete AV block, then you need the AV junction or the ventricular myocardium to take over the role of the pacemaker, generating a junctional or ventricular escape rhythm, respectively.
But there is the possibility that neither happens, and you get something like this:
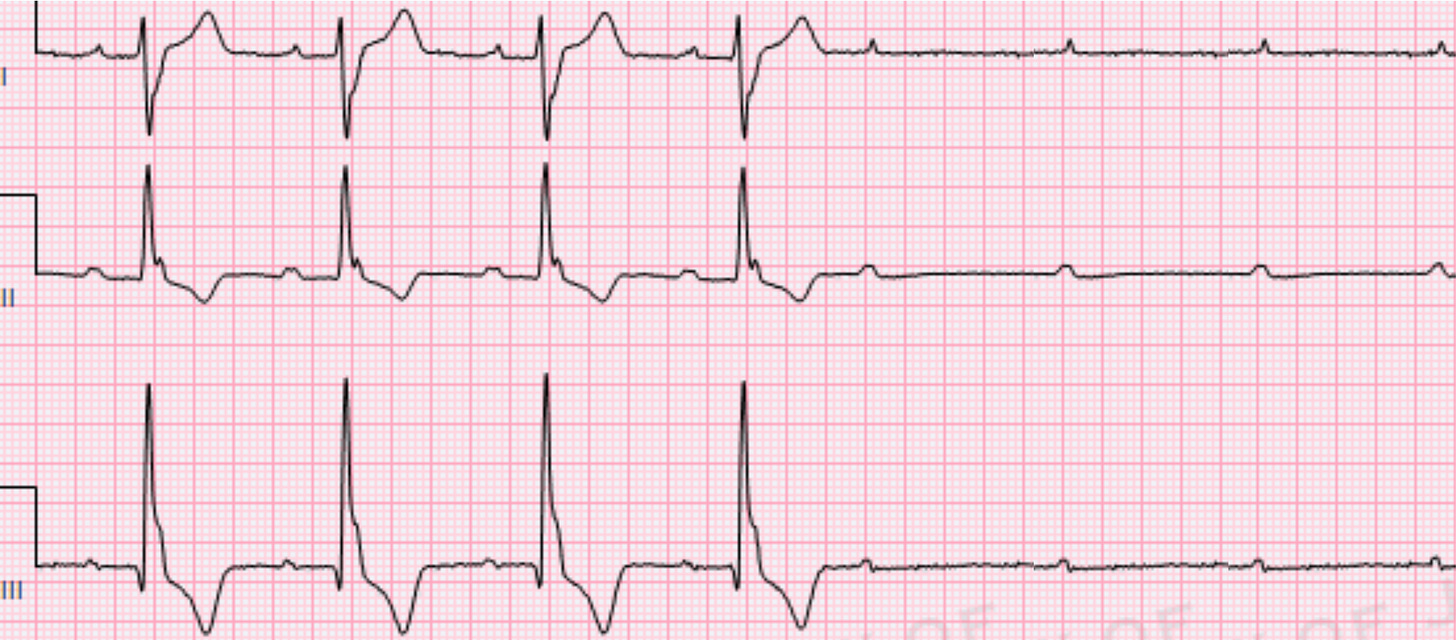
You see, there’s no ventricular depolarisation, meaning that there’s no cardiac output!
As this phenomenon was paroxysmal, it was effectively cardiac syncope (also known as Adam-Stokes syndrome²). The brain's lack of oxygen during these episodes could explain the patient's seizure-like symptoms.
Swiftly, the patient was transferred to the cardiac high-dependency unit. Temporary intravenous pacing was set up, soon replaced by a permanent pacemaker.
A Cardiology consultant handed me the ECG and said, “What do you see here?”. After I spent something like 5 minutes analysing the ECG wave-by-wave, I said, “Trifascicular block?”. “Yep”, he said, nodding his head.
That day remains etched in my memory. It wasn't just about identifying blocks on an ECG; it was about connecting theoretical knowledge to real-life scenarios. My learning had become relevant to what I was doing, which was essentially treating people.
That patient made it abundantly clear to me why learning about AV blocks, bundle branch blocks and fascicular blocks is important.
“Tying it (education) to solving a problem is, I think, very powerful for establishing relevance…”
- Elon Musk
What is attention
In "How We Learn" by Stanislas Dehaene³, the spotlight is on attention as the foundational pillar of learning.
To truly understand how attention works, let’s see how learning is coded in our brains. It's all about synapses, the bridges that let neuronal paths form. The brain isn't frivolous; it doesn't expend energy crafting synapses “just in case”. Instead, it strategically strengthens those synapses and pathways that have proven their worth through repeated activation.
What happens with attention? When you pay attention to something (a particular stimulus, say, the sight of the patient collapsing in front of you and the medical team’s reaction), although the stimulus might cease to exist, your neuronal path that fired when you experienced the stimulus continues to fire for a long time! This long-term potentiation is the signal that your brain needs to optimise this pathway.
Attention → long-term potentiation → neuronal path optimisation (i.e. learning)
The three attention systems
As per the American psychologist Michael Posner, there are at least three major attention systems:
Alerting - when you should pay attention
Orienting - what you should pay attention to
Executive attention - how to process the attended information
For the purpose of this post, I’d like you to pay “attention” (no pun intended) to the second attention system that your brain uses: orienting.
You are constantly bombarded with millions of stimuli, from smells in your room to the sensation of where your limbs are in relation to the rest of your body (proprioception) to your stomach sending signals to your brain that you should probably eat something. All these signals reach your brain constantly. So your brain has implemented a system to filter what is important and what isn’t.
And this is where the “why” comes in…
Knowing the “why” means you’ll pay attention
Knowing the “why” for learning something makes you pay attention to it.
This is why just-in-case learning is a total waste of time.
Find a problem first; this will give you a reason to care and pay attention.
Let generation make it clear to you why you need to learn something and what you need to learn exactly by struggling to solve a problem first.
So why do YOU learn ECG interpretation?
Perhaps you're still searching for your "why", that driving force that propels you forward. Don't wait for it to come to you. Go out, immerse yourself in the real world. Visit hospitals, engage with patients, and dive deep into genuine challenges. I guarantee you'll stumble upon countless scenarios that will ignite your passion for understanding ECGs and more.
For those who've already found their "why," I urge you to share it. Every one of us carries a unique tapestry of experiences. Too often, we downplay their significance, assuming they hold no value for others. But in sharing, we might just light a spark for someone else, offering them a perspective they hadn't considered.
This is why I write this newsletter.
Thanks for reading 😊
References
Dehaene, S. (2021) How we learn: The new science of education and the brain. UK: Penguin Books.
Sauer, William. “Chronic bifascicular blocks”. UpToDate, Dec 06, 2022.
Prutkin, Jordan. “ECG tutorial: Miscellaneous diagnoses”. UpToDate, Jun 08, 2022.

